Head Case: Living with Chronic Migraines
To the outside world, glamorous, model-pretty writer Tia Williams seemed to have it all. Inside, she struggled with ugly, crippling headaches.

There's me at 34, hooked up to a Demerol drip in a Turks and Caicos hospital, my soon-to-be ex-husband looking at me with unmistakable resentment. I have become a woman who ruins tropical vacations, vacillating between two states of being: obliterated on medication or catatonic from pain. I am a ghost who has disappeared almost totally into her disease.
While most people can look back on their lives against a backdrop of momentous occasions — a Sweet 16 here, a wedding there — mine is punctuated by debilitating, brain-crushingly violent migraine attacks. Here I am at 12, in the school cafeteria, focusing my gaze on a single potato chip, thinking, If I keep staring at it, if I just concentrate, I won't pass out from agony. Then at 22, new to New York City, interrupting my first sexy grown-up date to hide out in the bathroom, stabbing myself in the thigh with an injection of pain meds. Next, I'm 28, at a work lunch, struggling to act normal before stumbling outside to vomit on the street. And at my first book signing, in my hometown of D.C. — everyone I know is there — the pain tearing through my face like tiny Ginsu knives, my signature getting wonkier and wonkier, until I finally excuse myself and faint in the cookbook aisle on my way to the bathroom.
Over the years, I've tried it all. I've been to top migraine doctors, tested every new treatment — yoga, biofeedback, meditation, color visualization, and even Chinese medicine, which involved chugging down specially mixed herbal teas that tasted like incense-flavored sludge. Traditional migraine pills like Imitrex did zilch for me — it was like swallowing Skittles. Nothing helped, and eventually, without fail, my doctors gave up. I was labeled incurable, intractable — and I ended up at pain clinics, languishing in waiting rooms with recovering junkies and cancer patients, hoping that a shot of morphine would get me through the day.
The past six months have been a revolving door of weeklong hospital stays — me, on various IVs, waiting for the throbbing to break. I've had no social life. Even my closest friends have gotten bored ("Whatever, just take a Tylenol and come meet us!"), and potential boyfriends have lost interest because I couldn't keep dates. My 4-year-old daughter has worried over me like an adult, hyperaware of every telltale sign that I'm in pain. When I heard she was having meltdowns at preschool from the stress, my heart broke, a different agony than I normally experience but just as acute.
It was in this state that my new migraine doctor recommended neurostimulation therapy, an extreme surgery available to only the most hopeless chronic pain patients. The procedure came out of pacemaker technology from the late 1970s, the idea being that, instead of taking pills to regulate severe discomfort, you could use stimulation to override pain signals to the brain. Initially used to treat only back pain, over time neurostimulation has been shown to work for migraines, MS, and even depression. The procedure involves implanting tiny, mildly vibrating wires under the skin at the site of the pain (in my case, at each of my temples); the electrical impulses block the pain signals from reaching your brain. My doctor explained that, like something out of science fiction, the wires would run subcutaneously from my temples down each side of my neck, join at my upper back, stretch down the side of my body, and connect to the neurostimulator — like a matchbox-size battery power pack — implanted in my upper butt cheek. This is what would send the electric impulses to my temples. And — wait for it — I would adjust the intensity of the stimulation with a remote control. I would be a real-life bionic woman.
After my doc broke down the procedure, I searched her face for signs she was joking. I scanned the room for cameras. (Does ABC have an extreme-surgery reality show? I wondered.) But no, she was serious, and neurostimulation therapy was my only option. I was terrified. Was I going to move like a robot? Could I have an orgasm with this implant, or would it short-circuit the whole operation?
As I mulled it over, I realized that I'd be insane not to try it. Nothing — and I mean nothing — had ever worked. I already had zero quality of life. I had nothing to lose.
Get exclusive access to fashion and beauty trends, hot-off-the-press celebrity news, and more.
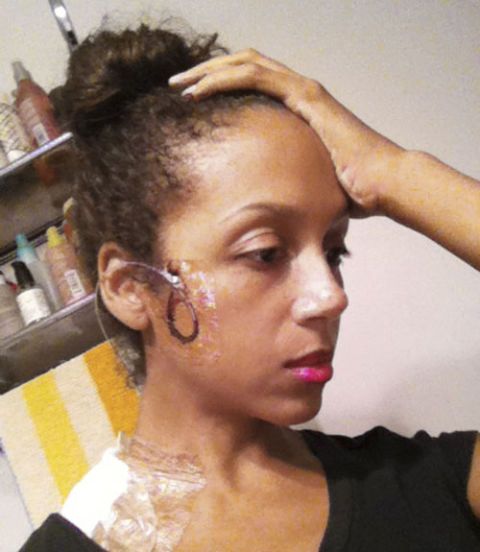
After I resolved to become bionic, I dove into the six-month-long, two-part approval process. First was the extensive psychiatric evaluation to make sure I wasn't "making up my condition," despite the busted capillaries in my nose caused by two decades of scrunching up my face in agony. But I was used to doctors second-guessing my pain. (Some assume you're a junkie seeking pills. Others, especially male doctors, write off migraines — which are suffered overwhelmingly by women — as a sort of female hysteria. In 10th grade, a doc actually told me that getting a boyfriend and going to more school dances might help me relax a bit and lessen the pain.) But the series of psych evaluations was nothing compared with the next hurdle: a weeklong trial to make sure the treatment would work. Instead of surgically implanting the actual neurostimulator, my doctor had me use a makeshift version: The leads, super-skinny wires with electrodes dotting the ends, were slid under my skin at the temples, with the thick wires connecting them to the mechanism left outside of my body. For a week, I walked around with blood-encrusted wires taped to the sides of my face and neck in thick loops, the neurostimulator perched on one shoulder under a mountain of gauze, looking like I'd just been tortured by a sadistic electrician. Children pointed, my mailman asked me if I'd been in a car accident. A concerned Hungarian barista sputtered, "Your face ... it looks ... hurting." Normally polished, I felt deformed. But there was something freeing in this. For the first time, I felt like my outside matched my inside.
More important, during the week of the trial, I felt better than I had in years. Every morning of the past year, I'd woken up and shaken my head a bit, trying to gauge not if I had a migraine, but how bad it was. Instead, almost every day that week, I was pain-free. The relief was, ironically, somewhat dizzying.
· ONE MONTH LATER, I had the actual surgery. When I awoke, I could barely move, my neck, temples, and back swollen and disfigured. My hair was shaved a bit above my ears, and I had stitches up the side of my face, lending me the look of an '80s-style face-lift patient. I never really thought of myself as a vain person, but when I first looked in the mirror, I dissolved into tears.
Then after about a week, the swelling went down and I healed. And miraculously, the migraines stayed at bay. There are inconveniences: I can no longer go through metal detectors (when I travel, I have to carry a little card with me officially explaining as much), and a couple times a week, I have to wear a charger belt over my butt for an hour, like a human iPad. I will live the rest of my life rigged up like C-3PO, and if I leave my remote in a cab or something, I'm screwed because it's a fortune to replace. On the other hand, my migraines have lessened considerably. I can now have dance parties with my daughter, who no longer gazes at me with concern. I can make it through a date without pill-popping, or work without having to fight Percocet-induced narcolepsy. The clarity is life-changing. I am bionic, hear me roar.
