The Coldness of Enduring Breast Cancer in a Covid-19 World
In June, breast cancer survivor Kai McGee went to the hospital for her annual mammogram and ultrasound. Now she has to decide the next steps in her treatment journey, an already-stressful process made worse by the isolation of Covid-19.

Around one in eight American women will be diagnosed with breast cancer in their lifetime, and each is so much more than a statistic. Every Monday during Breast Cancer Awareness Month, we'll be chronicling the journey of one Black mother and survivor as she navigates the uncertainty of breast cancer in these uncertain times.
When I was diagnosed in 2014 with stage II breast cancer, the world was not battling a pandemic. The enormity of hearing the words, “your tumor is malignant” is life altering—I can’t imagine hearing those words under the stress and isolation of a Covid-19 world.
Given all the unknowns about Covid, I felt nervous scheduling my annual breast mammogram and ultrasound in June, a routine I’ve followed for six years. I wondered if it would be safe to go to the hospital and how the protocol would be different. When the hospital called to confirm my appointment, I had to answer new questions including “Do you have any symptoms of Covid-19?” “Have you had a fever?” “Have you been exposed to anyone with Covid-19?” “Have you left the state?” I was told that I must wear a mask upon entry, that no one would be allowed to accompany me, that my temperature would be checked, and that I’d have to wear a face covering during the entire visit, which can last up to three hours.
When I arrived for my exam, the hospital parking lot was eerily empty. There was an attendant standing at the main entrance to take my temperature. Once I was deemed fever-free, I was required to sanitize my hands. I explained to the attendant that I only use natural sanitizer; she was visibly irritated and barked that I had to use the hospital’s. I explained that I am a cancer survivor, going for my annual cancer screening, and would rather not use their sanitizer but am happy to use my own. She finally conceded and let me proceed.
The mammogram waiting room without a pandemic is horrible. The mammogram waiting room during Covid-19 is hell. Every woman was masked up sitting in chairs strategically placed six feet apart, anxiously waiting to be called. There is usually lots of nervous chatter, but on this day there was deafening silence—the atmosphere cold, isolating, and more depressing than usual.
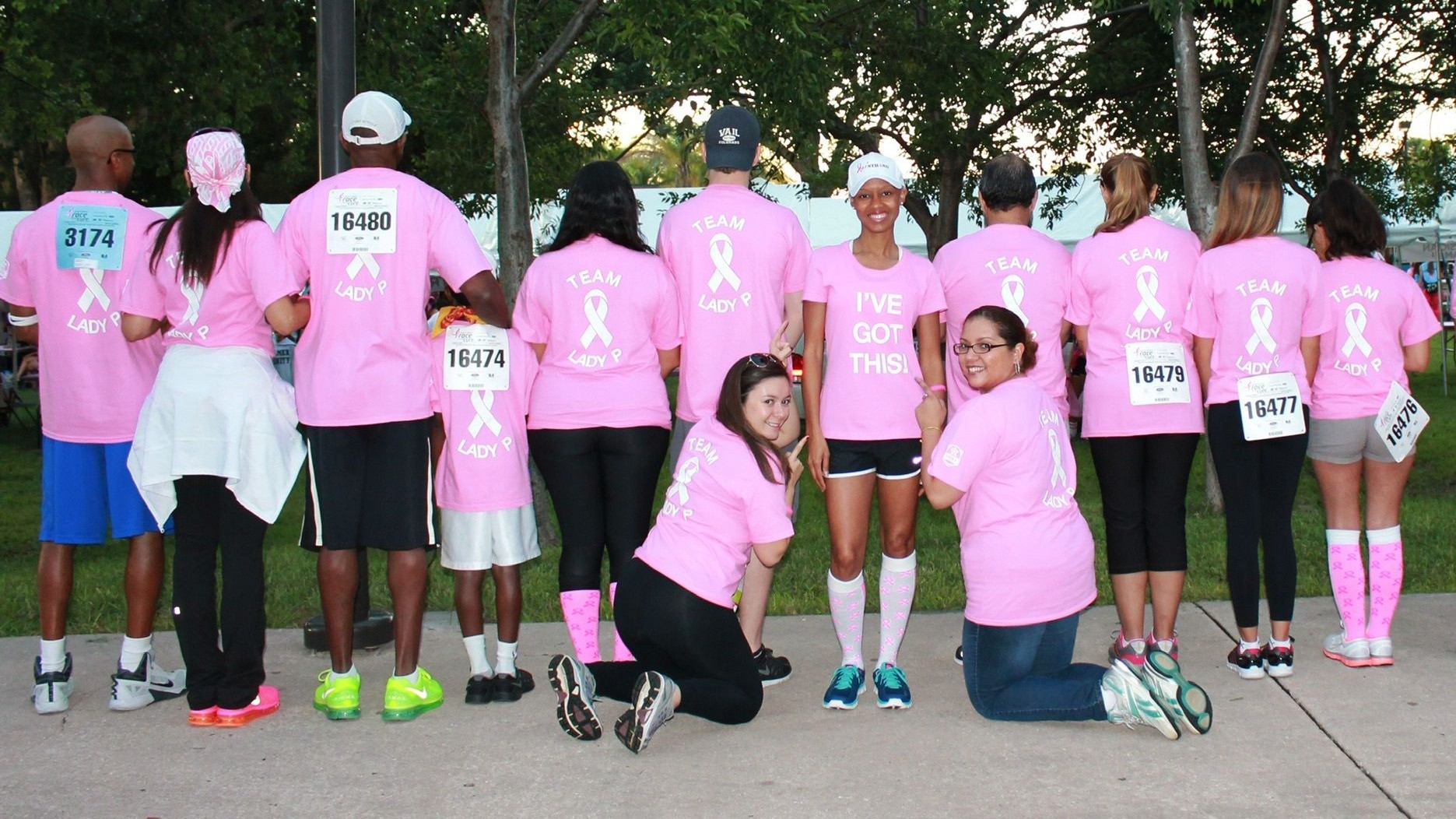
When the author (center, facing forward) was battling breast cancer in 2014, her friends and family were able to arrange a walk in her honor.
Covid-19 has made my follow up healthcare visits equally as challenging. After my routine breast exam in June revealed suspicious calcifications, I started meeting with countless medical professionals to chart a course of action. Shortly after my biopsy revealed that I have atypical ductal hyperplasia, medical professionals in my home state of Florida moved to telehealth visits and the hospitals halted all non-emergency surgeries. Fortunately, I was able to have my initial appointment with my breast surgeon in-person; all my follow up appointments have been via webcam.
My breast surgeon ordered an MRI of my chest and genetic testing for 48 types of cancer. Given my history of breast cancer, these tests were ordered to rule out any cancerous tumors or lesions that may have been undetected. The genetic test was saliva based and I was able to complete that at home: I followed the instructions, sealed the package, and dropped it at the overnight courier.
Get exclusive access to fashion and beauty trends, hot-off-the-press celebrity news, and more.
The MRI was a difficult process. Once again, I was masked up and alone. Due to the sentinel node dissection I had on my left side in conjunction with my breast cancer surgery in 2014, I can only have blood drawn from my right arm. My veins tend to play hide and seek, and, on this day, they were determined to hide. After several failed attempts, the nurse inserted the MRI dye through a vein in my hand. Even after numbing the area first, the pain was tremendous. Masked up, freezing cold, and in discomfort, I closed my eyes and hoped the process would end quickly. It did not. About an hour later I was desperate for fresh air, sunlight, and hugs from my son.
I had telehealth visits with two different breast reconstruction surgeons. They told me about the multiple surgeries, the breast expanders, the tubes, the drains, the pain, and the grueling process that is a bi-lateral mastectomy. I have endured unspeakable physical pain, trauma and recovery—I know I can handle whatever a mastectomy throws at me. So, I felt empowered to go with that procedure.
Masked up, freezing cold, and in discomfort, I closed my eyes and hoped the process would end quickly. It did not.
In a follow-up visit with the breast surgeon, she told me that there is still a reprieve on non-emergency surgeries, including the bi-lateral mastectomy that I was hopeful to undergo as quickly as possible. Hearing that left me deflated and anxious.
Yet another appointment was scheduled with my primary care doctor to take labs, check my overall health, and discuss my plan. I sat on my patio on a hot, sticky July evening, feeling such a sadness that none of these appointments include a mental health check-in. So many instructions, so many tests, so many methodical approaches to my physical body and not one visit included the question, “How are you, really?”
If any of the doctors had asked, I would have said, “I’m scared, frustrated, tired, worried.” I remember the PTSD I suffered after chemo ravaged me and left me with an 80-pound, lifeless body. The palpable sadness that I felt during and after my 2014 diagnosis and treatment started to feel heavy.
My telehealth visits continue, as do thoughts about going through a bi-lateral mastectomy alone in this unforgiving Covid-19 world. For the safety of hospital staff and patients, visitors are not allowed to accompany any patient for any reason. It became painfully clear to me that I would have to endure this major surgery without support. The simple act of a back rub, the timing of an inside joke, the energy of compassion transferred from a loved one’s hand to mine before being wheeled into surgery are all invaluable parts of the journey that I would have to forego.
For the first time through this process I’m questioning having the bi-lateral mastectomy. I don’t want to wait until Covid-19 is more controlled to have surgery, because no one knows when we’ll have a new normal or what it will look like. I’m not willing to endure the mental and emotional toll the isolation of going through a major surgery (and endless follow up appointments) alone entails.
I’ll continue to use this time until non-emergency surgeries open to reflect, meditate, and lean into my faith for the answer, trusting that I will be guided to do what is best for my future self.
Related Story

Kai McGee is a writer who frequently explores parenting, her journey through breast cancer, social-justice and self-care. She is currently working on her memoir. Connect with her via Instagram @onanaturalkai


