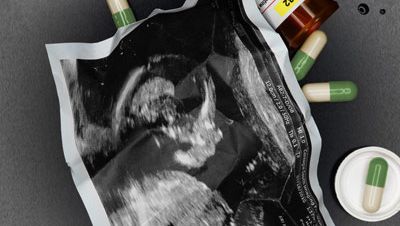
Suzanne, 29, was 33 weeks pregnant with her second child when she finally confided to her husband the dark thoughts she'd been having. "I hated being pregnant," Suzanne said. "So much so that I wanted to remove my stomach." Her husband blamed her hormones, but Suzanne knew it was something else. "I did not feel this way with my first pregnancy at all, so I figured I was upset because a close family friend had recently died," she said. "I kept waiting for those dark feelings to pass—but instead, they intensified." She went from being sad about the death to feeling like she wasn't connecting with her baby. When she began to feel anger toward her unborn child, she panicked. "The baby would kick at night, and I'd get mad," she says. At the time, she kept her feelings a secret, as she was too ashamed to admit them to anyone. "I had nothing to be sad about! I have a great husband, a great life," she says. "If I told people I could not get out of bed in the morning, they'd say, 'Why? What's the problem?'"
Depression was the problem. When Suzanne was finally diagnosed, a month after she gave birth to her child, the illness had become full-blown. "I knew about postpartum depression," Suzanne says, "but I'd never heard of depression during pregnancy." It's counterintuitive: Pregnancy is supposed to be the happiest time of a woman's life! But that expectation, combined with Suzanne's symptoms—fatigue, dark thoughts, inexplicable crying jags, a sense of hopelessness—left her guilty, confused, and, as it turned out, very sick. "The general feeling is, if you're not ecstatically happy about being pregnant, then you're obviously a terrible person who doesn't want your baby," says Dr. Gail Robinson, a professor of psychiatry who runs the Women's Mental Health Clinic at the University of Toronto. "As a result, women keep their depression a secret." And get progressively sicker.
Women are twice as likely to be affected by depression as men, and yet this illness, which will strike one out of five women in her lifetime, according to the National Institute of Mental Health, is hard to diagnose in the average woman, pregnant or not. That has much to do with depression's tricky symptoms: feelings of worthlessness, irritability, lethargy, as well as bouts of insomnia and sobbing spells. Everyone has a few bad days, but if these symptoms persist for a two-week period, chances are it's more than just feeling blue; it's a diagnosable illness.
And according to a slew of recent studies, depression occurs during pregnancy at an alarming rate. "Pregnancy used to be thought of as a honeymoon period from mood disorders—that the joy of having a baby plus the estrogen protected you," explains Dr. Sheila Marcus, codirector of the Women's Mental Health Program at the University of Michigan. "We now know that's not the case." In September 2009, the American College of Obstetricians and Gynecologists (ACOG) copublished a study with the American Psychiatric Association (APA) that found up to 23 percent of women experience depressive symptoms while pregnant. The same study found that 13 percent of women took an antidepressant at some point during their pregnancy, a number that has doubled since 1999.
If not treated—with psychosocial therapy, such as cognitive-behavioral therapy, or, in more severe cases, with medication—those symptoms will likely intensify after delivery. "For some women, postpartum depression is an extension of depression that started during pregnancy," Robinson says. That's what happened to Suzanne. Two months after her baby was born, she had a breakdown. "I burst into tears and kept telling my husband, 'I can't do this,'" Suzanne recalls. "I felt empty, and that made me feel horrendously guilty because I had this beautiful baby." That afternoon, Suzanne was diagnosed with postpartum depression and put on Wellbutrin.
Considering only one out of five women will seek treatment for her mood disorder while pregnant, Suzanne is representative of a large number of women who suffer their depression unknowingly and silently during pregnancy. Stigma is the biggest culprit. "You feel so ashamed," admits Suzanne. "You want to think that your mommy instinct will win out—and when it doesn't, you feel even worse."
The cruel symptoms of depression also make seeking help difficult. But several recent studies prove that staying depressed during pregnancy is actually dangerous for both the mother and her unborn child. "Women often think they're doing the best thing for their child by not getting treatment," says Dr. Healy Smith, a Manhattan-based reproductive psychiatrist. "It's tragic—if mom is sick, then the baby is impacted, too." That's because staying depressed or anxious while pregnant can actually harm the fetus. "Women run the risk of inadequate weight gain, which has been associated with low infant birth weight, and of missing prenatal appointments," Marcus says. "There's also the possibility of substance abuse, as untreated women are more likely to use alcohol during pregnancy." Other risks include the physiological effects of the illness: "When you're stressed, your body shifts into fight-or-flight mode and moves blood away from your placenta and toward your limbs and brain," Marcus says. "That's good if you need to run from a tiger; it's bad if you're growing a baby."
Get exclusive access to fashion and beauty trends, hot-off-the-press celebrity news, and more.
Thankfully, there are treatments that work. ACOG and the APA recommend non-pharmacological treatments, such as cognitive-behavioral therapy and talk therapy, as the first line of action for mild to moderate depression. That, in addition to stress management, sleep hygiene, and a supportive social network, can be effective. But for women who are severely depressed or anxious, these nonmedical approaches are often not enough. While studies up through 2005 found no rise in congenital malformations among women who took antidepressants while pregnant, a few studies since then have made links between antidepressants and heart defects, pulmonary hypertension, and low birth weights in newborns, all of which are being vigorously researched and debated in the scientific community. "The bottom line is that no decision is completely risk-free—whether you suffer the symptoms or take medication," says Dr. Vivien Burt, the director of the Women's Life Center at Resnick Neuropsychiatric Hospital at UCLA. "You have to talk with your doctor about what's right for you."
One thing is certain: Women who have depression in their family or have already been diagnosed with a mood disorder are at greatest risk for experiencing the illness during pregnancy. For these women, Burt recommends teaming up with their OB/GYN and a specialist to plan the safest pregnancy treatment before getting pregnant. That's exactly what Eliza, 33, did. She started taking Lexapro for severe anxiety in her mid-20s, but went off the pills when she and her husband decided to get pregnant. "I wanted to do everything I could to make this baby as healthy as possible," Eliza explains. "In my mind, that meant not taking a prescription." Though she carefully weaned herself off the prescription under the care of a reproductive psychiatrist, her anxiety re-emerged stronger than ever: "I felt totally overwhelmed, like I couldn't handle my job or my relationship, let alone my looming pregnancy." Her doctor suggested Celexa, as it had significantly more safety data with pregnant women than Lexapro, and Eliza agreed to go on the lowest dosage possible.
The irony is that many women decide to go off their medication before or during pregnancy in order to protect their child. "I'd been on antidepressants for anxiety prior to the pregnancy but worried about their effects on my unborn child," 33-year-old Kristy explains. "So I just stopped taking them." Already the mother of two, she didn't know then that abrupt discontinuation could result in a severe relapse: "In one study, 70 percent of women who went off their antidepressants while pregnant relapsed," Burt says. The swift and severe effects of Kristy's illness took her by surprise. "I went from being an on-top-of-everything working mom to someone who couldn't get out of bed," she says. She was so stunned by her feelings that she felt compelled to keep them a secret: "I called in sick to work, and then would force myself out of bed before my husband came home so he wouldn't know I'd been home all day," she says. "It got so bad, I didn't take my 2-year-old daughter to day care one morning because I was scared to be home alone. For the first time ever, I considered taking my own life and was actually afraid I'd act upon those thoughts." That's when Kristy told her husband everything. The following day, she saw a psychologist and a psychiatrist, then was put on Zoloft. "I decided in the end that the benefits outweighed the risks," she explains. "I couldn't imagine things getting worse. I wanted to salvage things before postpartum depression—or psychosis—set in."
Kristy's decision to return to medication while pregnant was due, in part, to the odds that her depression would spiral after her delivery. Sticking with her treatment, she gave birth to Lilah, a healthy girl, in mid-January. Meanwhile, Suzanne fully emerged from her postpartum depression when her daughter was 9 months old. And Eliza gave birth to a healthy girl almost a year ago; she stayed on a subclinical dose of antianxiety medication throughout her pregnancy under the supervision of her reproductive psychiatrist. "The question should never be, 'Should I take medication or not while I'm pregnant,'" says Robinson, "but rather, 'Should I be sick or should I be well?'"
Liz Welch is an ASME-award-winning journalist whose work has appeared in The New York Times Magazine, Life, Parade, and Inc. Her memoir, The Kids Are All Right (Harmony), is due out in paperback in September 2010.