The Waiting Game
For women in 28 states, mandated waiting periods are making abortions complicated, expensive, and nearly impossible.

Sarah, a 26-year-old with blue eyes and pink nails, wakes up before sunrise on the outskirts of Knoxville, Tennessee. Normally, she'd head to her outpatient rehab program, which she attends voluntarily every day for an addiction to prescription painkillers. But this Monday, she won't make it: She's got a doctor's appointment. She climbs into her weathered Nissan Maxima, drops her 3-year-old daughter Laela off at her mother's house, and makes the 45-minute drive to the Knoxville Center for Reproductive Health, which is located so close to the University of Tennessee campus that appointments aren't scheduled during home football games. Sarah parks her car and walks briskly past a group of pro-life protesters, which includes a couple of devoted regulars: two middle-aged men who've been protesting on this spot for over a decade.
Thirty-four women like Sarah have appointments today. It's a typical day for the clinic, but a not-so-typical one for the patients, who have to drive as long as eight hours from as far away as Kentucky and Mississippi to get there. When Sarah arrives, the waiting room is half-full of women fiddling with their phones or watching Rachael Ray on a TV screen. A couple speaks in Spanish. A toddler sleeps in the hallway. One young woman leans on her boyfriend and wipes away tears.
Sarah got pregnant during a drug relapse and is eight weeks along. She's no longer in touch with the father. Sober for only about four weeks now, she wants to focus on getting clean before having another child.
But when she called the clinic to make her appointment, she learned she would not be able to get the procedure right away—Tennessee is one of 28 states that now requires women to undergo a waiting period before having an abortion. Here, the mandatory wait is 48 hours. And here, as in about half the states with waiting periods, Sarah is also required to attend an in-person counseling session, meaning she has to make two separate trips to the clinic.
"They're just telling you to sit there and think about what you're about to do...do people think it's not hard enough as it is?"
Those two days play out like this:
Sarah's first appointment takes over four hours, most of which she spends, coincidentally, waiting. There's only one doctor at the clinic today, who has to split her time between this, another clinic, and another private practice. The staff is stretched thin.
First, Sarah undergoes a lab test verifying she is pregnant, along with an ultrasound. A staffer takes her medical history and checks in on how she's feeling emotionally. Under Tennessee law, a woman cannot be coerced into an abortion, so the staffer ensures that she is not. Sarah then watches a 15-minute video that details the risks associated with abortion and the aftercare. And as part of new legislation that took effect last July, a board-certified doctor conducts "counseling," which entails reading Sarah a state-approved script that informs her that abortion "constitutes a major surgical procedure." Further still, the state requires the doctor to inform her that a fetus can survive outside the womb 24 weeks after conception (despite the fact that there aren't any clinics in Tennessee that will perform abortions after 16 weeks). The doctor then must legally add that should Sarah decide to proceed with her pregnancy, there are services available to support her.
Get exclusive access to fashion and beauty trends, hot-off-the-press celebrity news, and more.
Only after all this can Sarah provide informed consent.

Sarah outside the Knoxville Center for Reproductive Health, where she sought an abortion
This script varies from state to state. In Indiana, women are told that "human physical life begins when a human ovum is fertilized." In Missouri, they receive a pamphlet declaring that "abortion will terminate the life of a separate, unique, living human being." In Louisiana, counseling includes a booklet that reads, "by 20 weeks gestation, the unborn child has the physical structures necessary to experience pain." Lawmakers have been known to borrow language from anti-abortion groups when they write these materials.
The next available appointment for Sarah's procedure is Friday, four days later. That means two more 45-minute drives, but also a special consideration: Sarah has to call her rehab program and inform a staff member that she has to miss another day. Rehab patients who miss Mondays and Fridays—prime drug binge days before and after a weekend, but also the primary days the Knoxville Center for Reproductive Health performs abortions—can be subjected to extra scrutiny by the addiction counselors. And because, for now, Sarah is unable to end her pregnancy, she will continue to have intense morning sickness, and have to miss additional sessions that week. Sarah is warned she could be discharged from her program if she misses more days without a valid reason.
For the next few days, Sarah alternates between worry and nausea. "The waiting period caused me to be sick longer," she says about morning sickness—but the additional emotional degradation also takes its toll. "They're just telling you to sit there and think about what you're about to do...do people think it's not hard enough as it is?"
Access to abortion is, despite the political chaos of recent years, a constitutional right.
But the net effect of these waiting periods—compounded with the slew of state laws that have closed clinics or made it impossible for them to continue to operate—has transformed abortion access into an uphill battle for women across the country. For many, abortion is no longer a viable option at all.
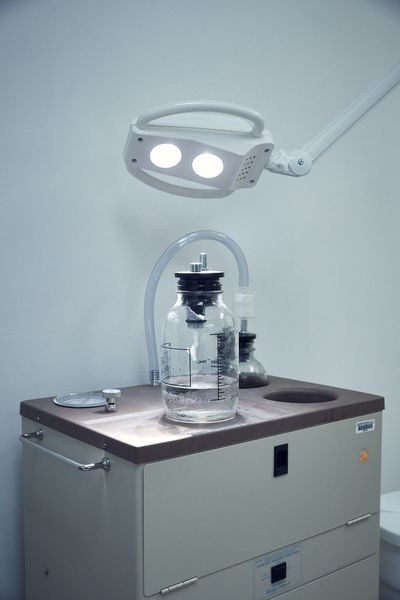
There are a number of concerns about the waiting period in particular. Not surprisingly, those most affected by waiting periods are poorer women, who may have driven across state lines to seek care and can't afford to make the trip again or stay overnight. In states that require two separate trips to a clinic, that's two days of missed wages, two days of childcare (most women who get abortions are already mothers), and two days of transportation.
There's also the slippery slope effect: In recent years, right-to-life groups have taken advantage of the waiting-period standard and aggressively targeted state legislatures to insist on longer and longer waiting periods. If the courts are okay with 24 hours, how about 48? Or 72? At least five states adopted new or longer waiting periods in 2015, preceded by two states in 2014. Six states now require women to wait 72 hours before getting an abortion, the longest in the country. Last year, according to Elizabeth Nash, senior state issues associate at the Guttmacher Institute, was "the most action we've seen around waiting periods in an incredibly long time."
In states that require two separate trips to a clinic, that's two days of missed wages, two days of childcare, and two days of transportation.
What's more, because abortion is a time-sensitive procedure, delays can mean increased medical risk. Bekki Vaden, a surgical assistant at the clinic in Knoxville, says she "quite often" sees women schedule appointments early enough in their pregnancies so that they can have what's known as a "medical abortion"—a combination of medications injected, taken orally or inserted vaginally. But by the time they are able to secure an appointment for the second visit, they are further along, which means a more invasive "surgical abortion" (in which suction is used to remove the contents of the uterus) is necessary. And once a woman crosses the second trimester, this procedure can be more painful, Vaden says, because the cervix must be dilated further and there's more tissue to remove.

Bekki Vaden, surgical assistant, in a room where abortions are performed. On the ceiling, a sign reads: You are Strong, You are Brave, You are Wise, You are Beautiful, You are Worthy
State by state, pro-choice activists are fighting back. In Florida, which passed a 24-hour waiting period last year, women's health advocates are suing, claiming the statute violates a woman's right to privacy under the state constitution—if a woman must wait and make an extra trip, she's more likely to have to disclose her medical condition to explain it.
Meanwhile, all eyes are on the Supreme Court, which on Monday is expected to hand down a decision on whether Texas' abortion restrictions are unconstitutional. The state has effectively shuttered at least 23 of its 41 providers in the last four years, forcing women to travel farther and farther distances to get an abortion. If left standing, the restrictions could reduce the number of clinics to a meager 10. While the case doesn't specifically address waiting period laws, the decision could greatly impact this kind of litigation going forward.
But while the legal battles play out, American women are forced to navigate the costly repercussions of abortion waiting periods.
"I have patients scared to death, in tears when they realize they must explain to an abusive partner why they are sneaking away twice."
Women like Suzy Dalton, 28, who was a nanny living in Huntsville, Texas when she became pregnant in 2014. Without health insurance at the time, and with the nearest Planned Parenthood some 50 miles away, she relied on condoms for contraception. "I don't think I'm the first one who'd been in that situation," she says.
Dalton has a genetic disorder that requires her to take medication that could cause complications were she to give birth. Even still, she has no interest in having children at this stage in her life, so she chose to exercise her constitutional right to an abortion.
But in the current political climate, her nearest abortion clinic is in Houston, an hour away. And because of Texas's 24-hour waiting period, she had to take two non-consecutive days off work. Dalton avoided telling the mother she worked for why, and felt guilty that she had to hide the truth. "Since I worked with kids, I didn't want to be seen as someone who didn't want kids of my own," she says. Dalton estimates that she lost about $200 in wages and spent $50-60 in gas to make the trip, in addition to the $250 for the abortion, which she says "decimated" her bank account. She had to rely on her credit card to cover basic living expenses.
For her first visit to the clinic, Vanessa, a 24-year-old student and part-time restaurant server in Florida, told her boss she had to help out family in West Palm Beach. (There are closer clinics, but she used to work at that facility and felt more comfortable there.) She also had to concoct elaborate lies to tell the father, now her ex-boyfriend, who worked with her at the same restaurant and strongly opposed her having an abortion, she says. (Because of privacy concerns, MarieClaire.com could not verify this account with the father.)
After her first appointment, she spent the next day afraid that her ex was going to find out the truth. "Having to sit there and wait, you just get very anxious," she says. The day after that, she made the eight-hour drive again, and told the restaurant she was sick. She worries about other women who are in more precarious situations, risking their employment and safety just to make that second trip. "It's tough for me now, and I can't imagine for somebody else," she says.
She's right to worry. Waiting periods can be especially traumatic for victims of domestic abuse. "I have patients scared to death, in tears when they realize they must explain to an abusive partner why they are sneaking away twice," says Kelli Cassini, a health counselor at the Knoxville clinic. Cassini, a domestic abuse survivor, has advised other women who fear for their physical safety—should a violent partner find out they had an abortion—on how the after-effects of the procedure mimics a miscarriage. She maintains that victims feel more at ease knowing a partner can't find out for sure.
Dr. Susan Dodd, 60, is the only full-time abortion provider in Knoxville. With a frank, soft Southern drawl, she explains that she had an illegal abortion in Knoxville in 1972 when she was 16—a year before Roe v. Wade, an experience she remembers as "terribly frightening and painful." That event influenced her decision to become an abortion provider, though she admits it's been a challenging career choice. She's just finished a seven-hour shift (having seen 34 patients) and is scarfing down a late 15-minute lunch before heading to another clinic, Planned Parenthood, to see more patients. Tomorrow morning she is scheduled to do a hysterectomy at her private practice, an OBGYN office, where she works three days a week in order to maintain the hospital admitting privileges Tennessee law requires abortion providers to have.
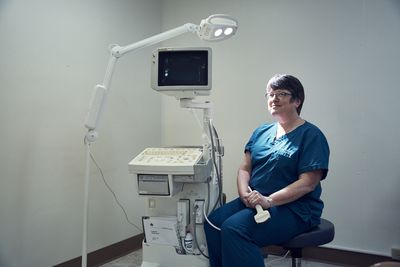
Dr. Susan Dodd in the second room for abortions at the Knoxville Center for Reproductive Health
When not racing back and forth between clinics, Dr. Dodd regularly meets with the FBI to discuss personal security measures. Her husband, a biology teacher at a local college, bought her a bulletproof vest she stows in the trunk of her car. They also keep a gun in the house, just in case. "If someone shoots me or whatever, it will probably be kind of hard to convince somebody else to take my place," she says.
If Dr. Dodd doesn't follow Tennessee's rigorous abortion practitioner requirements to the letter—if, for example, she's running late and has a nurse read the government script that constitutes informed consent—she could face a felony conviction and a year of jail time. That 10 minutes extra with each patient adds up to nine additional hours a week to her already tight schedule. She says she's never seen a patient change her mind because of the material she is required to read.
"If someone shoots me or whatever, it will probably be kind of hard to convince somebody else to take my place."
Of the 19 women who saw Dr. Dodd on Monday for their pre-abortion counseling, 16 return for abortions after the waiting period, including Sarah. (Privacy laws prevent the clinic from sharing what became of the other three patients.) Now nine weeks pregnant, Sarah opts for a less invasive medical abortion. This is her second abortion, she tells me, and it's much more painful than the first. Committed to staying sober, she refuses painkillers. The pain is so intense that it makes her sick, and she throws up repeatedly. She'd like to take a few days off to recover, but she's worried she'll lose her spot in rehab and decides to go back the next day.
A few months later, Sarah is still in rehab—proudly 108 days sober—and has also been hired as a full-time sales representative for an international trading company. Things are looking up. Still, it's easy for her to play the what-if game: What if she'd been kicked out of rehab? What if she didn't have the right to choose at all? She doesn't pause long to consider it. "I don't know where I'd be."
Dana Liebelson is a writer in Wyoming. Her journalism has been published in Mother Jones, HuffPost, The Atlantic, Marie Claire and Insider.
